Introduction:
Legg-Calve-Perthes Disease’ is a childhood hip disorder in which the blood supply to the ball of the hip joint (femoral head) is obstructed. This results in weakening of the bone of the femoral head which may extrude partially from the socket, lose it’s spherical shape, and, become flattened and irregular (Figure 1).
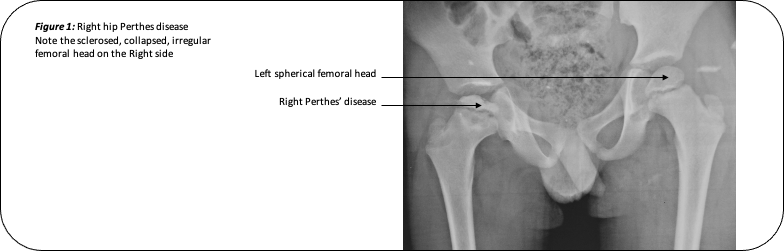
Perthes disease typically affects children between the ages of 4 to 10 years. It is 5 times more common in boys than in girls. It usually affects only one side, both sides are involved in only 10% cases.
Causes:
The exact cause is not known. In most cases, no underlying cause is detected. However many theories including role of genetic factors, increased clotting tendency of blood and hormonal imbalances have been proposed to play a role in the causation of Perthes’ disease.
Natural course:
Perthes Disease passes through four stages, each stage lasting several months. From the onset of the illness, it typically takes 1.5 to 2 years to heal completely.
Children in whom the spherical shape of the femoral head is preserved till healing occurs have good long term prognosis.
However, cases in which the femoral head is flattened and aspherical, arthritis of the hip joint may develop in early adult life.
Clinical features:
The most common symptom is a limp. It may be painless, or the child may complain of mild, intermittent pain in the groin, thigh or even knee. The affected hip may be stiff, i.e. less movement as compared to the opposite hip.
Treatment:
To start with, your doctor will get an X-ray both your child’s hip joints, to see what stage the disease is in and how severe it is. In some cases, an MRI might also be required.
The goal of treatment in Perthes disease, is to prevent extrusion and maintain the spherical shape of the ball of the hip joint during the natural course of the disease which lasts about 1.5 to 2 years. This would ensure good long term outcome.
To achieve that goal, treatment may be either non-operative or operative.
Non-operative treatment:
Non-operative treatment is effective in younger children (less than 6 years) with Perthes’ disease. This consists of:
– Rest to the joint: non weight-bearing, though difficult to enforce, is ideal
– Medications: as and when required, to reduce pain
– Physiotherapy: may be recommended to reduce hip joint stiffness
– Traction and hip spica cast application: may be recommended in cases where stiffness persists after above measure.
Operative treatment:
Non-operative treatment usually fails in older children (> 6 years old) and therefore, operative treatment is usually recommended in this age group. The surgery is aimed at preventing extrusion of the ball (femoral head) from the socket and thereby preserve the sphericity of the femoral head. The surgery is called containment surgery and can be done on the thigh bone (femoral varus-derotation-osteotomy) or pelvic bone (pelvic osteotomy).
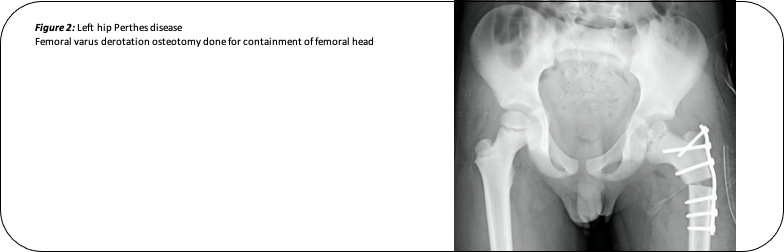
Prognosis:
Most children with Perthes Disease do well and return to normal activity. The outcome is better in children who are younger and have less severe involvement.
Long term outcome is directly correlated with shape of femoral head at healing. Children in whom the spherical shape of the femoral head is preserved till healing will have a good long term prognosis and hip joints which will last for a life-time.
In some children, it may not be possible to maintain the spherical shape of the ball despite all efforts. Such children may require further treatment, including surgery, when they are adolescents or adults. Some may develop arthritis in adult life which needs Total Hip Replacement surgery.
Once the disease has healed fully, most children are able to play sports. During treatment however, your doctor will probably advise you to avoid sports so as not to place too much stress on the hip while it is healing.
This article is contributed by Dr Sandeep Vaidya, Paediatric Orthopaedic Surgeon, Pinnacle Orthocentre Hospital, Thane. Dr Vaidya is also available for consultations at BJ Wadia Children’s Hospital, Mumbai; Ajit Scan Centre, Kalyan; and Ace Children’s Hospital, Dombivli. For more information, call 7028859555/ 8879970811/ (022)25419000/ 25429000 OR email drsvvaidya@gmail.com.
