CASE 1:
12 years old girl, a known case of Neurofibromatosis Type 1, presented with shortening and deformity of Left leg since birth. Her Xrays revealed Left Congenital Pseudarthrosis of Tibia. She had undergone six surgeries elsewhere but her pseudarthrosis had failed to heal.
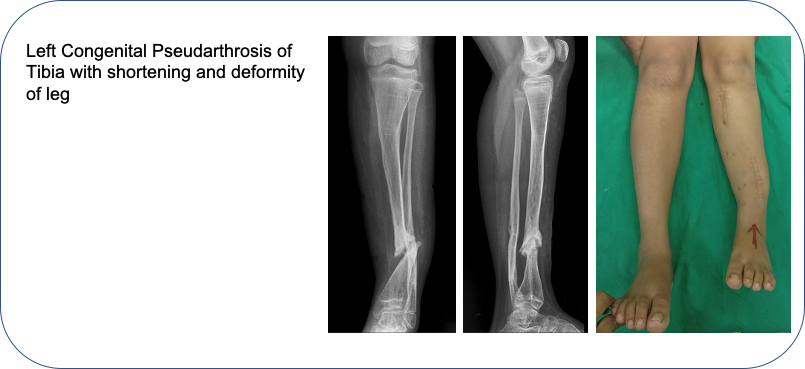
She underwent surgery by our new comprehensive protocol for pseudarthrosis excision, fixation with rod and plate, and bone grafting.
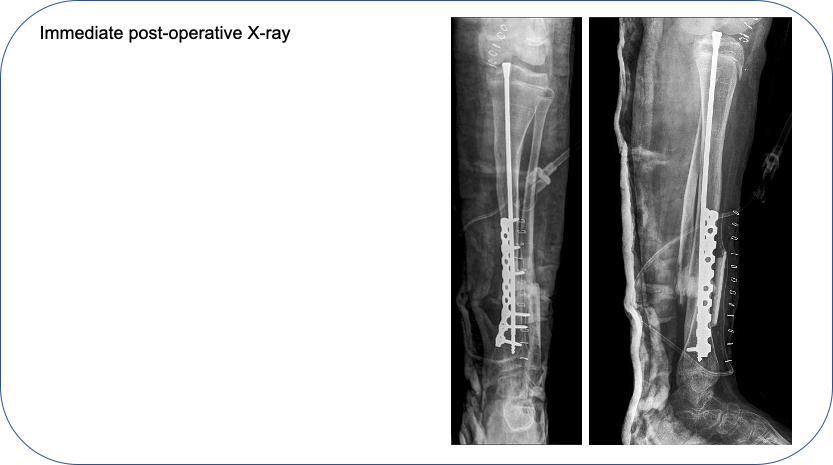
At two years post-operative, the pseudarthrosis has healed and deformity is corrected.
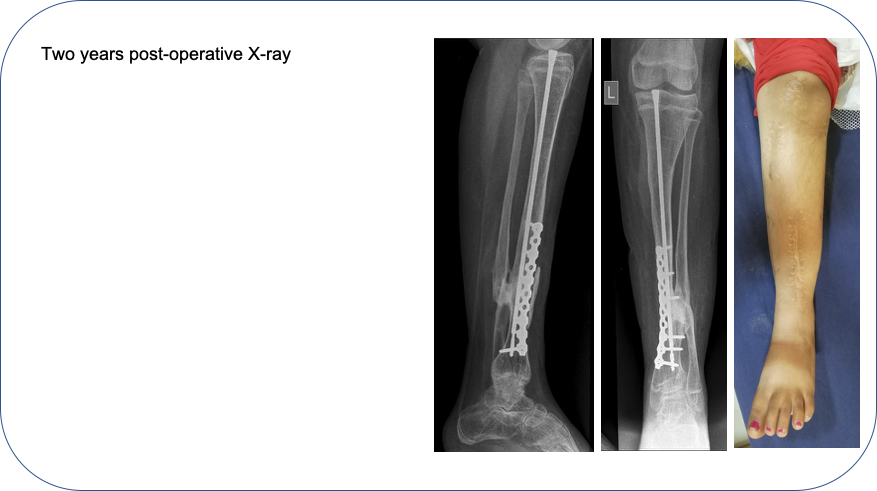
CASE 2:
A one year old female child presents with antero-lateral bowing of Right tibia bone.
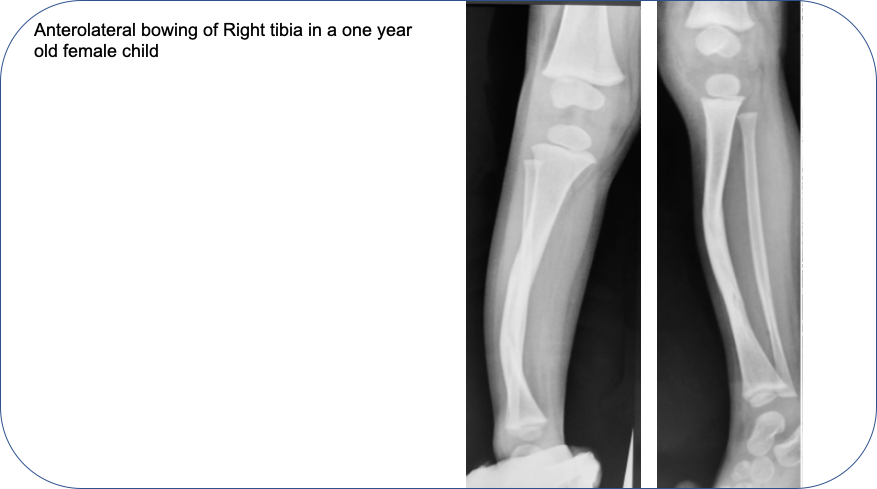
The lesion progressed to a frank fracture (CPT) by age 2 years.
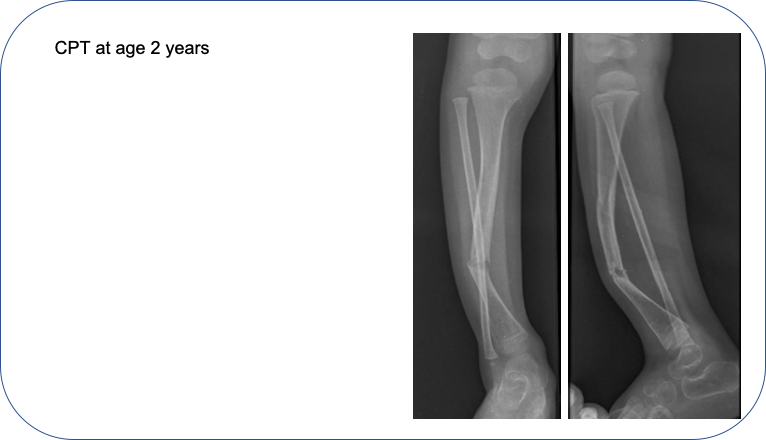
The child was operated by our new comprehensive protocol.
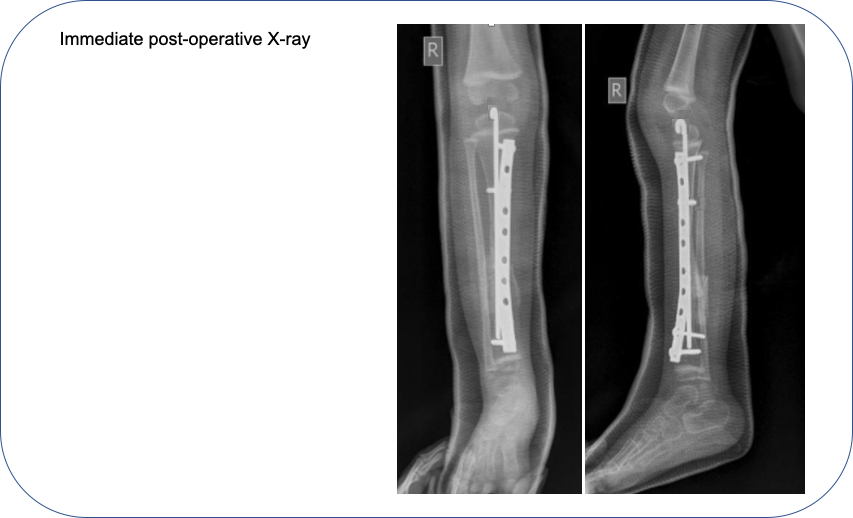
At 2 years post-operative, the pseudarthrosis has solidly healed, deformity if fully corrected and child is fully functional.
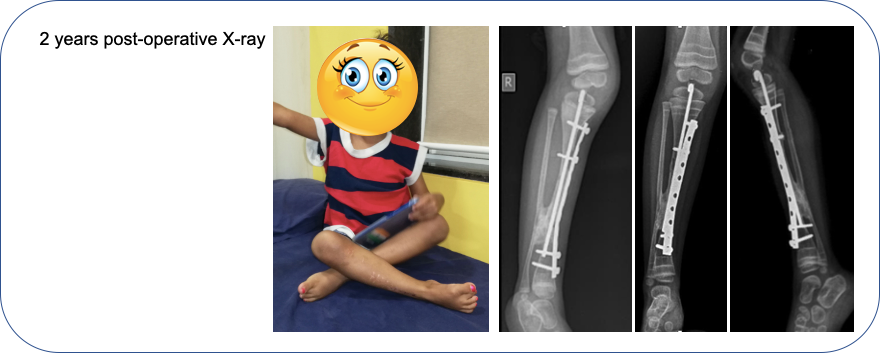
DISCUSSION:
Congenital Pseudarthrosis of Tibia (CPT) is an extremely rare condition and occurs in 1 in 1,50,000 children. In 50% cases, CPT is associated with a genetic condition called Neurofibromatosis Type 1.
In this condition, the leg bone (tibia) is usually bowed at birth but progresses to frank fracture (pseudarthrosis) by age of 2 years.
Treatment of CPT is always surgical. Traditional treatment methods were associated with significant difficulty in achieving union, and, multiple surgeries were often needed for achieving union.
However, in recent years, we have been using a new treatment protocol with excellent success rate. The results of our technique have been peer-reviewed and published in the Indian Journal of Orthopaedics (see Reference below).
REFERENCE:
Vaidya Sandeep V, Aroojis A, Mehta R, Agashe MV, Dhawale A, Bansal AV, Sarathy K. Short Term Results of a New Comprehensive Protocol for the Management of Congenital Pseudarthrosis of the Tibia. Indian J Orthop. 2019 Nov-Dec;53(6):736-744. doi: 10.4103/ortho.IJOrtho_155_19. PMID: 31673175; PMCID: PMC6804390.
This article is contributed by Dr Sandeep Vaidya, Paediatric Orthopaedic Surgeon, Pinnacle Orthocentre Hospital, Thane. Dr Vaidya is also available for consultations at BJ Wadia Children’s Hospital, Mumbai; Ajit Scan Centre, Kalyan; and Ace Children’s Hospital, Dombivli. For more information, call 7028859555/ 8879970811/ (022)25419000/ 25429000 OR email drsvvaidya@gmail.com.
